Vascular Destabilization and Pericyte Detachment are Mediated by hIAPP Aggregation in Transgenic Mice.
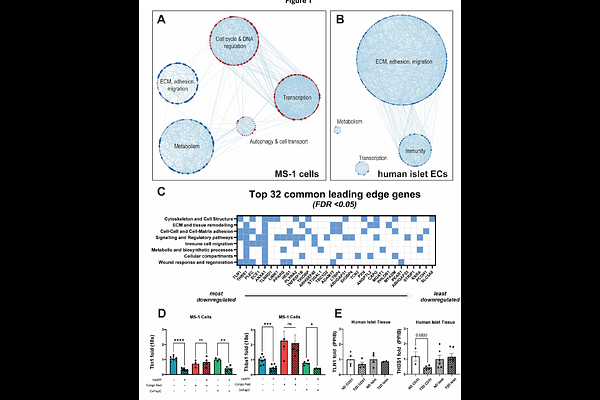
Vascular Destabilization and Pericyte Detachment are Mediated by hIAPP Aggregation in Transgenic Mice.
Koepke, J.; Mateus Goncalves, L.; Andrade Barboza, C.; Aplin, A. C.; Hackney, D. J.; Gharib, S. A.; Mohn, O.; Teng, M.; Castillo, J. J.; Almaca, J.; Hull-Meichle, R. L.
AbstractAims/hypothesis: Human islet amyloid polypeptide (hIAPP) deposition is a common feature of type-2 diabetes (T2D). Previous studies have demonstrated hIAPP-mediated endothelial cell (EC) dysfunction and inflammation, but little is known about islet microvascular stability or pericyte function in hIAPP-containing islets. This study investigates how islet endothelial cells and pericytes are influenced by hIAPP aggregation. Methods: Bulk RNAseq and qPCR were conducted on hIAPP or vehicle treated MS-1 cells and bead-purified human islet CD31+ cells from donors with or without T2D to determine how islet ECs respond to hIAPP exposure. Confocal imaging of living pancreatic slices obtained from hIAPP transgenic mice was conducted to evaluate the effect of hIAPP deposition on islet pericyte function and vasomotor responses. Results: hIAPP-treated MS-1 cells and ECs purified from T2D islets demonstrate downregulation of leading-edge genes associated with extracellular matrix and cell adhesion pathways. Pericytes from hIAPP-expressing mouse islets appear detached from underlying endothelial cells, which was associated with impaired vasomotor responses to constrictive or dilatory stimuli. Conclusions/interpretation: hIAPP induces vascular destabilization by downregulating mRNA of key extracellular matrix and cell adhesion molecules in ECs, likely promoting the breakdown of EC-EC and EC-pericyte coupling. hIAPP disrupts EC-pericyte connections, and pericyte detachment ultimately impairs pericytes' ability to modulate capillary diameter without impairing intracellular Ca2+ dynamics. Our data suggest that amyloid deposition compromises EC health and survival by altering islet microvascular morphology, stability, and function. This, in turn, may disrupt islet microvascular stability and exacerbate endocrine cell dysfunction in T2D.